
Telemedicine Reimbursement
and Regulations
Providers entering this emerging field should be vigilant of new policies, regulations, and other changes.
By Max Reiboldt, CPA

The potential uses of technology in the healthcare marketplace continue to expand in this era of innovation. Telemedicine has grown exponentially over the past few years as increasing demand for access to patients and cost constraints become more prominent.
Telemedicine is the delivery of healthcare through communications technology between providers and patients with a focus on improving access to care. The technological developments in telemedicine allow for the expansion of the scope of services and the provision of cost-effective care to patients. Telemedicine enables healthcare facilities the ability to reduce hospital admissions, readmissions, and emergency room volume by treating patients with chronic conditions who may otherwise be unable to seek treatment or manage their conditions effectively. Patients with minor ailments or those needing follow-up visits can also use telemedicine when an in-person visit is unnecessary. Additionally, telemedicine facilitates better patient care by connecting patients to specialists they often otherwise are unable or not as readily able to access. This lack of access especially applies to rural and other shortage areas.
Though telemedicine promises to expand access and improve the quality of care for patients, providers have traditionally hesitated to adopt its use due to the uncertainty of reimbursement and compliance concerns. Compliance-related regulations and requirements for telemedicine reimbursement vary among federal and private payers. Further, states differ on how telemedicine is covered and reimbursed. Thus, providers entering this emerging field should be vigilant of new policies, regulations, and other changes.
 Medicare and Telemedicine Medicare and Telemedicine
Medicare regulations for telemedicine reimbursement include stipulations on the location of the patient and provider, eligible types of providers, and method of telemedicine care delivery. Common terms in telemedicine include the originating site, which refers to the patient’s location at the time of service, and distant site, referring to the provider’s location at the time of service. The regulations determining the eligibility for Medicare originating sites include a county outside of a Metropolitan Statistical Area (MSA), which are determined by the Census Bureau and a recognized Health Professional Shortage Area (HPSA). Further, patients must also be located in an authorized originating site at the time of service. Under Medicare, authorized originating sites are physician or practitioner offices, hospitals, critical access hospitals (CAHs), rural health clinics, FQHCs, hospital-based or CAH-based renal dialysis centers, skilled nursing facilities (SNF), and community mental health centers. Medicare patients and providers participating in a Next Generation ACO are eligible for the CMS Telehealth Expansion Waiver. The waiver eliminates any geographic restrictions for telemedicine and also allows patients to be located in their own homes. This allowance is normally not authorized for Medicare reimbursement, in addition to any of the previously mentioned eligible sites.
Medicare also specifies which types of providers are authorized to bill and collect reimbursement. Currently, eligible practitioners include physicians, nurse practitioners, physician assistants, nurse-midwives, clinical nurse specialists, nurse anesthetists, clinical psychologists and social workers, registered dieticians, and nutritionists.
 There are three categories of telemedicine: store-and-forward, real-time interactive, and remote patient monitoring. Only telemedicine encounters rendered in a real-time interactive audio-video format are eligible for reimbursement. Store-and-forward encounters (where patient records, images, videos, etc., are collected and forwarded electronically to a provider for evaluation) are reimbursable only in Alaska and Hawaii. There are three categories of telemedicine: store-and-forward, real-time interactive, and remote patient monitoring. Only telemedicine encounters rendered in a real-time interactive audio-video format are eligible for reimbursement. Store-and-forward encounters (where patient records, images, videos, etc., are collected and forwarded electronically to a provider for evaluation) are reimbursable only in Alaska and Hawaii.
Billing Codes
Medicare telemedicine services are billed using CPT codes with the appropriate modifier. A “GT” modifier must be used in addition to the CPT code to bill for services. If located in Hawaii or Alaska and using a store-and-forward method of care, the “GQ” modifier should be used instead. Also, the place of service (POS) muse be “02” to indicate the billed service was furnished as a telehealth service from a distant site. Originating sites will also be eligible to charge a separate facility fee that is billed under HCPCS code Q3014 as a Part B payment. For 2018, the CMS allowable telehealth originating site facility fee is $25.76. If all the requirements are met, Medicare will reimburse providers at the same rate for telemedicine services as for comparable in-person services. This provision is very important as providers may now realize the economic value proposition of telemedicine as it becomes as financially viable as it is operationally viable.
A sample offering of Medicare Telehealth Services – Calendar Year 2018 is illustrated below.
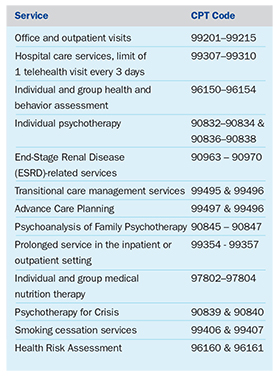
Medicaid and Telemedicine
Medicaid coverage for telemedicine is much more varied as states have extensive control over how to structure and administer their Medicaid telemedicine policy. Most regulations can be grouped into major areas, such as eligible modalities of telemedicine, eligible locations for service, eligible providers, obtaining consent for treatment, and online prescribing.
Currently, 48 states and the District of Columbia provide some form of reimbursement for live-video telemedicine services. Thirteen states will reimburse for store-and-forward telemedicine services. Twenty-two states reimburse for remote patient monitoring (RPM), limited to specific conditions. RPM is a form of telemedicine where health data (vital signs, weight, blood pressure, etc.) is consistently collected from a patient using digital technologies and transmitted to a provider to use in the management of health or disease. Finally, there are eight states whose Medicaid programs will reimburse for all three forms of service: Alaska, Arizona, Hawaii, Illinois, Minnesota, Mississippi, Missouri, and Washington.

Different restrictions and allowances for telemedicine exist among states’ Medicaid programs regarding several major areas of policy and regulation. As with Medicare, states can determine eligible locations for both the originating and distant site. For the originating site, 24 states have no restriction on the patient location, and 40 states allow the patient’s home as an originating site. Unlike Medicare, Medicaid is limiting the geographic restriction requirements with only six states having a specific geography or distance between the provider and patient. The types of providers vary in who are eligible to bill and be reimbursed for telemedicine services. Fifteen states’ Medicaid programs presently cover any healthcare provider to practicing telemedicine, while four states limit coverage to only physicians.
In general, reimbursement for Medicaid covered telemedicine care must satisfy federal requirements of efficiency, economy, and quality of care. Medicaid calls for the awareness of many more compliance-related issues tied to reimbursement than for Medicare due to the variance of regulation by state. These rules and regulations are rapidly changing as states continue to pass legislation regarding telemedicine, such as potential reimbursement for additional costs encompassing technical support, transmission charges, and equipment. Therefore, it is essential to remain vigilant of all potential and upcoming changes in the states related to telemedicine to qualify for maximum reimbursement.
Private Payers and Telemedicine
Commercial payers have perhaps been the most aggressive in reimbursing for telemedicine visits in recent years. Some are steadily broadening coverage through partnerships with telemedicine service companies. Twenty-nine states and D.C. have enacted telemedicine parity laws that mandate private payers to reimburse comparably as they would for in-person medical treatment. Eight states have proposed parity laws and are awaiting legislative action. Under such parity laws, coverage and restrictions still vary by state, but live-video telemedicine care is always covered to some extent.
The top five commercial payers—Aetna, Cigna, Blue Cross Blue Shield, Humana, and United Healthcare—all offer some form of coverage for telemedicine, even in states where coverage is not legally required, i.e., where there is no parity law. Telemedicine coverage is thus dependent on policy. For example, a Blue Cross Gold-Plan may cover telemedicine services while a Bronze-Plan might not. Many large private payers are conducting telemedicine pilot programs to test cost-saving benefits and care outcomes.
Advertisement. Click on image to visit advertiser's website. Story continues below.

|
Reimbursement rates from private payers depend on state policy and negotiated rates with providers. Some states mandate private payers to reimburse for telemedicine at the same amount as in-person care, but most states leave the determination of rates up to the payers. That said, a majority of commercial payers will still reimburse at the same rate as in-person visits. As with Medicare billing, most commercial payers require the billing of telemedicine services with the “GT” modifier, along with the correct CPT codes. Notwithstanding these commonalities, it is always important to verify with payers on their specifics regarding billing.
Compensation Models
In the majority of telemedicine arrangements, the distant site both bills and collects, not the provider performing the services. Therefore, the distant site must compensate the provider separate of billings, which is done via three models: flat rate per consultation or work relative units (wRVUs), hourly rate, and coverage stipend for availability. For the flat rate model, the provider is paid a predetermined amount for a consultation, and payment is tied to CPT code reimbursement. If the rate per consultation is $120, the provider would receive $120 in compensation regardless of the length of the consultation. On a flat rate per wRVU model with each wRVU worth $50 and the provider bills CPT 90832, which has a wRVU of 1.5, the provider will be compensated $75. An hourly rate model compensates the provider based on the amount of time spent providing consultations and the requirement of submission of a time sheet. With an hourly rate of $120, a provider performing telemedicine services for half a day (four hours) would be compensated $480. The model for coverage availability is similar to a call coverage arrangement in that the provider is compensated for being available, regardless of performing consultations. The provider would be required to be available for coverage for 24 hours and would be compensated a daily rate with or without providing consultations.
Looking Forward
Telemedicine is a rapidly growing area within the provider-patient relationship and is expected to expand access to care and create more cost-effective healthcare delivery. It has increased from 250,000 patient users in 2013 to an anticipated 7 million patient users by 2018. As health networks expand to encompass multiple states through clinically integrated networks and reimbursement shifts to value-based payments, health systems and providers are looking to telemedicine to improve the value of care and drive down costs. The greatest challenge with the adoption of telemedicine is that regulations, such as those related to reimbursement for specific services and the amount of reimbursement, are not yet standardized from state-to-state. Remaining aware of upcoming changes to policies and other compliance is vital as this emerging method of care-delivery evolves. To avoid risks and pitfalls, successful implementation of telemedicine programs start with and require understanding and compliance with all federal and state legal requirements and regulations. As a result, any provider or provider organization contemplating telemedicine as a service should adopt the following strategies:
- Ascertain the best applicable care continuum model category.
- Understand state and federal reimbursement realities.
- Educate all applicable staff and providers of the telemedicine clinical protocols.
- Inform all administrative associates of the rules and regulations for billing and charge capture.
- Complete both a tactical and strategic plan for the delivery of telemedicine services.
- Consider all cutting-edge technology for the delivery of telemedicine services.
- Complete pro forma financial projections for the delivery of telemedicine services.
- Check with the professional liability insurance carrier to assure complete and adequate coverage.
- Complete appropriate licensure arrangements for the delivery of telemedicine services.
- Educate performance regularly and include overall quality of care delivery.
 Max Reiboldt, CPA, is president/CEO of Coker Group with 44 years of total experience, the last 25 years specifically focused on healthcare. He has experienced firsthand the incredible changes of healthcare providers, which uniquely equips him to handle strategic, tactical, financial, and management issues that health systems and physicians face in today's evolving marketplace. Max Reiboldt, CPA, is president/CEO of Coker Group with 44 years of total experience, the last 25 years specifically focused on healthcare. He has experienced firsthand the incredible changes of healthcare providers, which uniquely equips him to handle strategic, tactical, financial, and management issues that health systems and physicians face in today's evolving marketplace.
|


 Medicare and Telemedicine
Medicare and Telemedicine There are three categories of telemedicine: store-and-forward, real-time interactive, and remote patient monitoring. Only telemedicine encounters rendered in a real-time interactive audio-video format are eligible for reimbursement. Store-and-forward encounters (where patient records, images, videos, etc., are collected and forwarded electronically to a provider for evaluation) are reimbursable only in Alaska and Hawaii.
There are three categories of telemedicine: store-and-forward, real-time interactive, and remote patient monitoring. Only telemedicine encounters rendered in a real-time interactive audio-video format are eligible for reimbursement. Store-and-forward encounters (where patient records, images, videos, etc., are collected and forwarded electronically to a provider for evaluation) are reimbursable only in Alaska and Hawaii. 


 Max Reiboldt, CPA, is president/CEO of Coker Group with 44 years of total experience, the last 25 years specifically focused on healthcare. He has experienced firsthand the incredible changes of healthcare providers, which uniquely equips him to handle strategic, tactical, financial, and management issues that health systems and physicians face in today's evolving marketplace.
Max Reiboldt, CPA, is president/CEO of Coker Group with 44 years of total experience, the last 25 years specifically focused on healthcare. He has experienced firsthand the incredible changes of healthcare providers, which uniquely equips him to handle strategic, tactical, financial, and management issues that health systems and physicians face in today's evolving marketplace.